Many patients come to the clinic with similar concerns:
“Doctor, I just have dandruff.”
“The skin around my nose keeps peeling and never goes away.”
“It gets red again as soon as I stop the medication.”
“I’ve tried so many shampoos, but it keeps coming back.”
The truth is, many of these cases are not just dandruff or cosmetic irritation, but seborrheic dermatitis—a chronic, relapsing skin condition closely related to sebum production, skin microbiota, immune response, and modern lifestyle factors.
This condition is not life-threatening. However, if underestimated, improperly treated, or self-managed with long-term medication misuse, it can cause persistent discomfort for years: itching, reduced confidence, prolonged poor skin condition, indirect hair loss due to inflammation, dependency on topical medications, and even complications from corticosteroid overuse.
Medical advice: Seborrheic dermatitis is not dangerous—but ignoring it can be very troublesome.
I. What is Seborrheic Dermatitis?
Seborrheic dermatitis is a chronic inflammatory skin condition that mainly affects areas rich in sebaceous glands:
- Scalp
- Forehead
- Eyebrows
- Sides of the nose
- Behind the ears
- Beard and mustache area
- Central chest
- Upper back
- Armpits, groin, under the breasts (in some cases)
Typical features include:
- Red or inflamed skin
- White, yellow, or greasy scales
- Mild to moderate itching
- Burning or stinging sensation
- Recurrent flare-ups
This is a chronic condition that can be controlled, but rarely “completely cured” permanently.
II. Why Does It Occur?
If you hear claims like “due to liver heat,” “bad blood,” or “vitamin deficiency,” be cautious.
Seborrheic dermatitis is a multifactorial condition.
1. Overactive sebaceous glands
Excess oil creates a favorable environment for inflammation.
Common in:
- Adolescents
- Young adults
- Oily skin types
- Males (in some groups)
2. Overgrowth of Malassezia yeast
This is a normal skin microorganism. When it overgrows or the body reacts excessively, it triggers inflammation and scaling.
In simple terms: it’s not a “dangerous fungal infection,” but an imbalance of the skin microbiome.
3. Impaired skin barrier
Skin becomes more vulnerable when damaged by:
- Harsh cleansing
- Over-exfoliation
Irritating cosmetics
- Dry weather
- Chronic stress
4. Stress – an underestimated trigger
Flare-ups often occur during:
- Deadlines
- Exams
- Sleep deprivation
- Work pressure
- Emotional stress
The skin cannot speak—it expresses distress through inflammation.
III. Symptoms by Location
1. Scalp
Most common site.
Symptoms:
- Heavy dandruff, flaky patches
- Itching
- Red scalp
- Scales sticking to hair roots
- May spread to forehead, neck, behind ears
Many people “treat dandruff for years” without properly addressing seborrheic dermatitis.
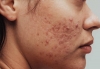
2. Face
Common areas:
- Nasolabial folds
- Eyebrows
- Forehead
- Mustache area
- Around ears
Symptoms:
- Persistent redness
- Fine scaling
- Burning sensation when using skincare
- Increased irritation with excessive products
3. Chest and upper back
Red patches with thin scales, sometimes arc-shaped or merging into larger areas.
4. Skin folds
Armpits, groin, under breasts: may appear moist and red, easily mistaken for fungal infection or intertrigo.
IV. Is It Contagious?
No.
You cannot transmit it through contact, sharing objects, or close proximity.
Do not let a skin condition become a psychological burden.
V. How Is It Different from Dandruff?
Simple dandruff may just be mild scaling.
However, if you have:
- Red scalp
- Persistent itching
- Frequent recurrence
- Spread to forehead or behind ears
- Greasy scales
…it is likely seborrheic dermatitis.
Dandruff can be just the “tip of the iceberg.”
VI. Diagnosis
Diagnosis is mainly clinical, performed by a dermatologist.
Conditions to differentiate from:
- Psoriasis
- Atopic dermatitis
- Tinea corporis
- Rosacea
- Contact dermatitis
When necessary, tests may include:
- Fungal examination
- Skin biopsy
- Supporting laboratory tests
VII. Treatment Approach
Modern treatment focuses on targeting the mechanism, not just using strong medication.
1. Scalp treatment
Shampoos containing:
- Ketoconazole
- Zinc pyrithione
- Selenium sulfide
- Ciclopirox
- Piroctone olamine
- Treatment depends on severity.
2. Face and body
May include:
- Topical antifungals
- Barrier-repair creams
- Appropriate moisturizers
3. Corticosteroid use
May be used short-term under medical supervision.
Overuse—especially on the face—can cause:
- Skin thinning
- Telangiectasia (visible blood vessels)
- Steroid acne
- Dependence
- Rebound flare-ups
Strong medication used incorrectly becomes harmful.
VIII. Why Does It Keep Recurring?
Five common reasons:
- Treating only flare-ups, not maintaining control
- Frequently switching products
- Chronic stress and sleep deprivation
- Hidden corticosteroids
- Misdiagnosis
IX. Long-term Care Tips
Sleep before 11 PM if possible
Manage stress
Wash hair regularly but not excessively
Use gentle cleansers
Avoid scratching
Choose simple, non-irritating skincare
Follow up regularly if prone to recurrence
X. When to See a Doctor Immediately
Severe scalp redness
Increased hair loss
Persistent facial redness and burning
Oozing or crusting
Severe itching affecting sleep
No improvement after months of self-treatment
Dependence on topical medications
XI. Doctor’s Perspective
Patients often seek “quick fixes.”
Good doctors focus on “long-term control strategies.”
That is the difference between symptom relief and proper treatment.
Seborrheic dermatitis requires discipline, understanding, and proper monitoring—not a miracle cure.
XII. Conclusion
Seborrheic dermatitis is a very common chronic skin condition that significantly affects appearance and quality of life. However, it can be effectively controlled with:
- Accurate diagnosis
- Mechanism-based treatment
- Proper skincare
- Stable lifestyle
If you have persistent dandruff, redness around the nose, eyebrow scaling, or recurrent scalp itching, don’t just keep changing shampoos—consult a dermatologist.
Many skin problems don’t require strong medication—just the right approach.
Professional consultation:
Dr. Doan Thi Bich Van, MD (Specialist Level I) - Dermatologist - Hoan Hao General Hospital